Make an Appointment: (339) 707-5236 | info@integrativepsychology.com
integrative psychology, PC
Cognitive Behavioral Therapy for Anxiety: What to Expect

Anxiety doesn’t just live in your head, it shows up in racing thoughts, tight shoulders, and sleepless nights. If you’ve been searching for a treatment that actually works, you’ve likely come across cognitive behavioral therapy for anxiety. CBT has decades of research behind it, and for good reason: it gives you practical tools to change the thought patterns and behaviors that keep anxiety running the show.
At Integrative Psychology, our experienced clinicians combine CBT with other evidence-based approaches to treat the whole person, mind and body. Our practice focuses on active, collaborative therapy where you’re not just talking about your problems but learning concrete skills to manage them. This integrative model means CBT often works alongside techniques like biofeedback and mindfulness-based interventions when a more comprehensive approach serves you better.
This article walks you through what CBT for anxiety actually involves: how it works, the specific techniques therapists use, and what you can expect from treatment. Whether you’re considering therapy for the first time or exploring options after other approaches haven’t helped, you’ll leave with a clear picture of how CBT can help you regain control over your anxiety, and what the process looks like from session one through lasting change.
Why CBT matters for anxiety
Anxiety disorders affect over 40 million adults in the United States, making them the most common mental health condition in the country. Yet despite how widespread anxiety is, many people suffer for years before finding treatment that actually creates lasting change. Cognitive behavioral therapy for anxiety stands out because it doesn’t just help you feel better temporarily; it teaches you specific skills that rewire the patterns keeping anxiety alive.
The research backing CBT for anxiety
Studies consistently show that CBT produces measurable improvements in anxiety symptoms within 16 to 24 sessions for most people. Research published by the National Institutes of Health demonstrates that CBT matches or outperforms medication for many anxiety disorders, with one critical difference: the benefits persist long after treatment ends. When you stop taking anti-anxiety medication, symptoms often return. When you complete CBT, you keep the tools.
The effectiveness spans different types of anxiety. Whether you’re dealing with generalized anxiety, panic disorder, social anxiety, or specific phobias, CBT has demonstrated efficacy across the board. This isn’t therapy based on hunches or outdated theories; it’s grounded in decades of clinical trials and neuroimaging studies showing actual changes in brain activity patterns after treatment.
CBT teaches your brain new pathways, not just new thoughts.
What sets CBT apart from other approaches
Traditional talk therapy often focuses on exploring your past and understanding where your anxiety comes from. CBT takes a different route. It concentrates on the present moment: what thoughts fuel your anxiety right now, what behaviors maintain it today, and what you can change starting this week. You spend less time analyzing childhood experiences and more time practicing concrete techniques that interrupt the anxiety cycle.
CBT is also time-limited and structured. You’re not signing up for years of open-ended sessions. Most people see significant improvement within three to four months of weekly meetings. Each session has a clear agenda, homework assignments that reinforce what you learn, and measurable goals you track together with your therapist.
Another distinguishing factor is the collaborative nature of treatment. Your therapist acts more like a coach than an advice-giver. You work together to identify patterns, test new strategies, and adjust the approach based on what produces results for you specifically. This active participation accelerates progress because you’re building skills you can apply independently.
Why timing matters for starting CBT
Anxiety tends to worsen when left untreated. What starts as worry about specific situations often spreads to more areas of your life. You begin avoiding more activities, your world shrinks, and the patterns become more entrenched. Starting CBT earlier in this progression means you have fewer compensatory behaviors to unlearn and can prevent anxiety from limiting your life further.
That said, it’s never too late to benefit from CBT. Even if you’ve lived with anxiety for decades, the techniques still work. Your brain maintains neuroplasticity throughout your life, which means it can still form new patterns and responses regardless of how long the old ones have been in place. People who’ve struggled with anxiety for years often report that CBT was the first treatment that gave them practical tools they could actually use when anxiety spiked.
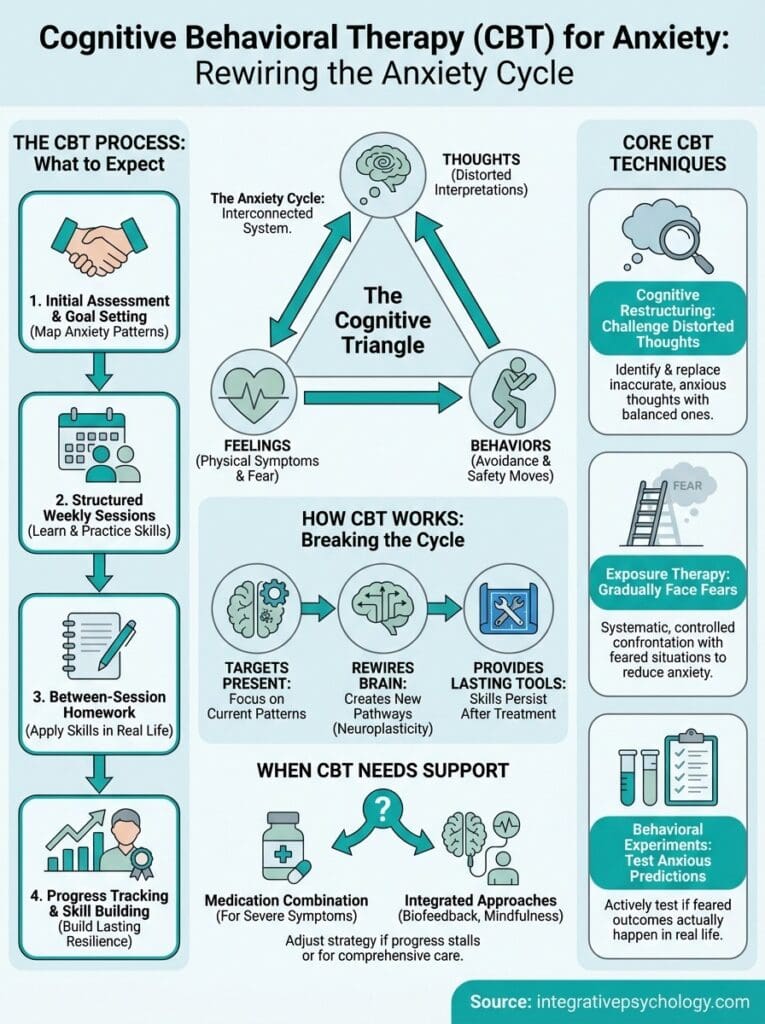
How CBT works for anxiety
Cognitive behavioral therapy for anxiety operates on a straightforward principle: your thoughts, feelings, and behaviors are interconnected, and changing one element shifts the entire system. When anxiety takes hold, your brain interprets normal situations as threats, which triggers physical symptoms and protective behaviors that actually reinforce the fear. CBT targets this cycle at multiple points simultaneously, giving you leverage to interrupt patterns that have become automatic.
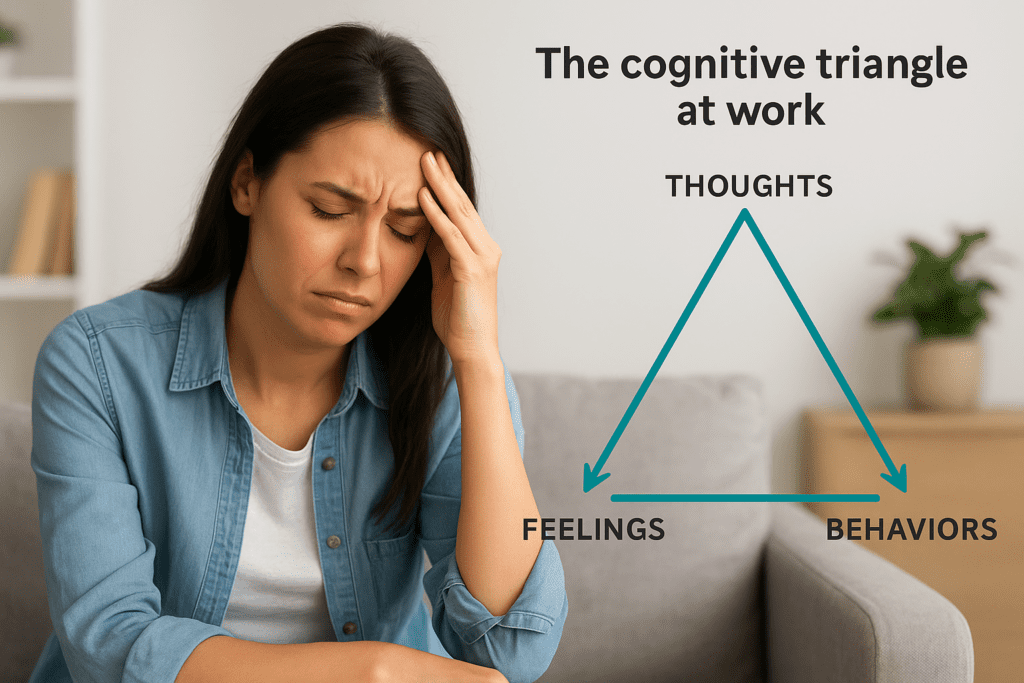
The cognitive triangle at work
Your thoughts about a situation directly influence how you feel and what you do next. If you think “I’m going to embarrass myself” before a presentation, your body responds with physical anxiety symptoms like rapid heartbeat and sweating, which the nervous system turns on whenever there is a perceived threat, even if just emotional. You then might avoid the presentation or rush through it, which confirms your belief that these situations are ‘dangerous’ (even if just emotionally dangerous or unpleasant). CBT helps you identify these unhelpful cognitive distortions (thoughts that don’t match likely, or balanced outcomes) and replace them with more accurate interpretations.
The process involves examining the evidence for and against your anxious thoughts. When you believe “everyone will judge me,” your therapist guides you to consider concrete data from past experiences. Most often, you’ll discover that your predictions don’t align with what actually happens. This evidence-gathering isn’t about positive thinking; it’s about seeing situations more clearly without the anxiety filter distorting your perception.
Anxiety convinces you that your worst-case predictions are facts, not fears.
Breaking the cycle through behavior change
Thoughts alone don’t maintain anxiety. Your behavioral responses play an equally critical role. When you avoid situations that trigger anxiety, you feel immediate relief, which teaches your brain that avoidance ‘works’. But this short-term solution strengthens anxiety long-term by preventing you from learning that the feared outcome rarely occurs.
CBT systematically reverses this through exposure. You gradually face anxiety-provoking situations in a controlled way, starting with less threatening scenarios and building up. Each successful experience rewrites your brain’s threat assessment. Your amygdala (the brain’s alarm system) learns to distinguish between actual danger and false alarms, reducing its automatic activation over time.
Behavioral experiments form another core component. Instead of just talking about whether your anxious predictions are accurate, you test them in real situations. If you fear people will think you’re stupid for asking questions, you might deliberately ask questions and observe what happens. These experiments provide firsthand evidence that challenges anxiety-driven beliefs more powerfully than logic alone ever could.
What to expect in CBT for anxiety
Walking into your first cognitive behavioral therapy for anxiety session often feels different than you might imagine. There’s no couch, no extended silence waiting for you to open up. Instead, your therapist greets you as a collaborator who will help you build specific skills through structured sessions with clear objectives. Most people feel relieved by this approach because it removes the ambiguity about what therapy involves and how progress happens.
The initial assessment and goal-setting
Your first session focuses on understanding your anxiety patterns in detail. Your therapist asks about specific situations that trigger anxiety, physical symptoms you experience, thoughts that run through your mind during anxious moments, and behaviors you use to cope. This isn’t small talk or general discussion about your childhood; it’s targeted information-gathering that maps exactly how anxiety shows up in your daily life.
Together, you identify concrete, measurable goals for treatment. Instead of vague aims like “feel less anxious,” you might target “attend social gatherings without leaving early” or “sleep through the night without worry spirals waking me up.” These specific goals let you track real progress and know when treatment is working. Your therapist also explains the CBT model, showing you how thoughts, feelings, and behaviors connect in your particular anxiety cycle.
The structure of typical sessions
Each session follows a predictable format that maximizes your time. You start by reviewing homework from the previous week, discussing what worked and what obstacles you encountered. Your therapist then introduces new concepts or techniques relevant to your current challenges, and you practice them together during the session before trying them independently.

Sessions usually last 45 to 50 minutes and occur weekly for most people, though some start with twice-weekly meetings if symptoms are more severe or if they want to progress faster. You receive homework assignments after each session, which aren’t busywork but essential practice that accelerates your progress. These assignments might include thought records, behavioral experiments, or exposure exercises that help you apply what you learned when anxiety actually strikes.
Real change happens between sessions, not just during them.
On average, treatment is relateively brief, and may last 16 to 24 sessions on average for many anxiety disorders, though you may notice improvements much sooner. Some people feel better after just a few sessions, while others need extra time to solidify new patterns. Your therapist adjusts the pace based on your progress and specific needs.
Core CBT techniques your therapist may use
Your therapist draws from a toolkit of proven techniques during cognitive behavioral therapy for anxiety, selecting strategies that match your specific symptoms and circumstances. These methods work together to target different components of your anxiety cycle, giving you multiple ways to interrupt patterns that have felt automatic. Understanding these core techniques before you start therapy helps you recognize what’s happening in sessions and why certain exercises matter for your progress.
Cognitive restructuring
This technique teaches you to identify and challenge the unhelpful, automatic negative thinking patterns that fuel anxiety. Your therapist guides you through examining thoughts that arise during anxious moments, questioning whether they reflect reality or catastrophic predictions your anxious mind generates. You learn to spot common distortions like mind reading (assuming you know what others think), fortune telling (predicting negative outcomes with certainty), and all-or-nothing thinking that eliminates middle ground.
The process involves writing down anxious thoughts and systematically evaluating the evidence for and against them. When you believe “I’ll definitely fail this test,” you examine past performance, preparation level, and actual probability rather than emotional probability. Your therapist then helps you develop balanced alternative thoughts that acknowledge uncertainty without defaulting to worst-case scenarios.
Anxious thoughts feel true because they’re loud, not because they’re accurate.
Exposure therapy
Facing feared situations gradually forms the backbone of lasting anxiety reduction. Your therapist creates an exposure hierarchy with you, ranking anxiety-provoking situations from least to most threatening. You start with scenarios that generate manageable discomfort and systematically work toward more challenging ones, staying in each situation long enough for your anxiety to naturally decrease without escape or avoidance.

Exposure happens both in imagination and real life. You might visualize a feared scenario while practicing relaxation techniques before attempting it in reality. Each successful exposure teaches your brain that the feared or worst-case outcome doesn’t automatically materialize, and that you can tolerate temporary discomfort without catastrophe. This relearning process can permanently weaken anxiety’s grip because you gather concrete evidence that contradicts your fears and learn that these fears can be challenged and approached differently.
Behavioral experiments and activity scheduling
Your therapist designs specific tests to challenge anxiety-driven beliefs through real-world experience. If you fear asking for help makes you appear incompetent, you deliberately request assistance and observe actual reactions. These experiments provide data that logic alone cannot, showing you directly whether your anxious predictions hold true.
Activity scheduling addresses the withdrawal patterns anxiety creates. When you avoid activities that once brought satisfaction, your mood drops and anxiety strengthens. Your therapist helps you schedule specific activities that provide accomplishment or pleasure, gradually rebuilding the behavioral foundation that anxiety eroded. This technique proves particularly effective when anxiety has narrowed your life significantly.
CBT for different anxiety presentations
Cognitive behavioral therapy for anxiety adapts its techniques based on your specific diagnosis and symptom patterns. While the core principles remain consistent, your therapist tailors the approach to address the unique ways anxiety manifests in your life. Understanding how CBT targets different anxiety presentations helps you recognize which strategies will likely form the foundation of your treatment plan and what outcomes you can expect based on your particular struggles.
Generalized anxiety disorder (GAD)
Treatment for GAD focuses on breaking the chronic worry cycle that keeps your mind spinning through worst-case scenarios across multiple life domains. Your therapist teaches you to recognize when you’ve shifted from productive problem-solving to unproductive worry spirals, then guides you through techniques to redirect this mental energy. You may practice scheduled worry time (confining worry to specific periods rather than letting it dominate your day) and develop skills to tolerate uncertainty rather than attempting to control every possible outcome.
CBT for GAD also addresses the physical tension that accompanies constant worry. You learn progressive muscle relaxation and other somatic techniques that reduce the body’s stress response, which then decreases the mental fuel available for worry. Your therapist helps you challenge the belief that worrying prevents bad outcomes, replacing this pattern with evidence-based planning and acceptance of what lies outside your control.
Panic disorder and agoraphobia
Your treatment targets the fear of panic symptoms themselves rather than just external situations. CBT helps you understand that panic attacks, while terrifying and extremely uncomfortable, actually pose no actual danger. You practice interoceptive exposure, which means deliberately triggering mild physical sensations similar to panic (like spinning to create dizziness) in safe conditions, teaching your brain these sensations don’t lead to catastrophe.
Therapists use cognitive restructuring to challenge catastrophic interpretations of body sensations. When you feel your heart racing, anxiety convinces you that something’s medically wrong. Treatment teaches you to recognize these as anxiety symptoms, not danger signals, reducing the fear that amplifies panic into full attacks.
Panic attacks feel dangerous, but the feeling itself is the threat, not what it warns against.
Social anxiety and performance anxiety
CBT addresses the excessive self-focus and mind-reading that fuel social anxiety. Your therapist guides you through exposure to social situations you’ve been avoiding, starting with less threatening interactions and building toward scenarios that trigger stronger anxiety. You practice attention training that shifts focus from internal monitoring (how you appear) to external engagement (what’s actually happening around you), which naturally reduces self-consciousness and anxiety during social interactions.
Getting the most from CBT between sessions
Cognitive behavioral therapy for anxiety doesn’t stop when you leave your therapist’s office. The real transformation happens during the other 167 hours of your week when you practice what you’ve learned in actual anxiety-provoking situations. Your therapist acts as a guide who teaches you skills, but you build lasting change through consistent application between sessions. Most people who see dramatic improvements report that homework assignments and between-session practice made the biggest difference in their recovery.
Completing your homework assignments consistently
Your therapist assigns specific exercises for a reason: they directly address the patterns maintaining your anxiety right now. When you complete thought records, exposure tasks, or behavioral experiments as assigned, you significantly accelerate your progress. Research shows that people who consistently do homework improve twice as fast as those who skip assignments or complete them halfheartedly.
Treat these assignments as seriously as you would physical therapy exercises after an injury. Schedule specific times for homework completion rather than hoping to fit them in when convenient. Most assignments take 15 to 30 minutes, and completing them immediately after sessions while the material remains fresh often produces better results. If you struggle with particular assignments, bring that obstacle to your next session rather than avoiding the work entirely.
Tracking patterns and progress
Keeping written records of your anxiety symptoms, thoughts, and situations helps you identify patterns your memory alone misses. Use a simple notebook or smartphone app to document when anxiety spikes occur, what triggers them, and which techniques you tried. This data gives you and your therapist concrete information for adjusting your treatment approach and shows you tangible evidence of improvement over time.
Progress in therapy rarely feels linear, but your records reveal the downward trend anxiety hides from you.
Regular tracking also builds your awareness of early warning signs, letting you intervene before anxiety escalates into full panic or avoidance. You begin noticing the subtle thought shifts or physical sensations that precede anxiety spikes, giving you opportunities to apply your CBT skills when they’re most effective.
Your therapist may also administer well-researched symptom and mood assessments throughout treatment for even more data about your progress and any areas that continue to need targeted approaches.
Practicing techniques in real situations
Reading about cognitive restructuring or exposure won’t reduce your anxiety; you must apply these techniques when anxiety actually hits. Start practicing in lower-stakes situations before attempting your biggest fears. When you feel mild anxiety, challenge the anxious thought immediately using the evidence-gathering method your therapist taught you. This real-time application strengthens neural pathways faster than any amount of discussion during sessions.
Accept that initial attempts will feel awkward and uncomfortable. Your new responses compete with years of automatic anxiety reactions, so expect some failures along the way. Each practice attempt builds skill, even when the outcome isn’t perfect and your therapist is there to help you learn and integrate these new ways of thinking, feeling and behaving
When CBT is not enough or not a fit
Cognitive behavioral therapy for anxiety works exceptionally well for most people, but it doesn’t solve every anxiety problem for everyone. Sometimes you need additional support alongside CBT, or a different approach entirely fits your situation better. Recognizing when treatment isn’t producing the results you need allows you to adjust your strategy rather than blame yourself for not improving fast enough. Your therapist should regularly evaluate progress with you and discuss alternatives when CBT alone falls short.
Signs CBT alone isn’t sufficient
If you’ve completed 16 to 20 sessions of quality CBT with minimal improvement in your anxiety symptoms, something needs to change. You might still experience the same frequency of panic attacks, continue avoiding situations at the same level, or find that anxious thoughts dominate your day despite practicing cognitive techniques. These patterns suggest you need additional interventions rather than more of the same approach.
Severe depression alongside your anxiety often limits CBT’s effectiveness because motivation and concentration required for homework assignments become nearly impossible. Similarly, active substance use typically interferes with learning and applying CBT skills. Your therapist might recommend addressing these issues first before continuing anxiety-focused CBT, or treating them simultaneously through integrated treatment.
CBT teaches skills, but other conditions can block your ability to learn them.
Undiagnosed medical conditions sometimes masquerade as anxiety or worsen existing anxiety symptoms. Thyroid disorders, heart arrhythmias, and sleep apnea all produce physical sensations identical to anxiety. If your anxiety doesn’t respond to CBT despite good homework completion, consider medical evaluation to rule out underlying health issues that require different treatment.
When medication becomes necessary
Some people benefit from combining CBT with medication, particularly when anxiety severely disrupts daily functioning. Medication can reduce symptom intensity enough that you can actually engage with CBT techniques and complete exposure exercises. Research shows that for severe anxiety disorders, the combination often produces better outcomes than either treatment alone, especially in the short term.
Alternative approaches worth considering
Trauma-focused therapies like EMDR work better than standard CBT when past traumatic experiences drive your anxiety. Dialectical Behavior Therapy (DBT) adds crucial emotion regulation skills that basic CBT doesn’t emphasize, making it particularly effective for anxiety complicated by emotional dysregulation. Acceptance and Commitment Therapy (ACT) offers a different philosophical approach that some people find more helpful than CBT’s thought-challenging focus.
At Integrative Psychology, Our team of experienced clinicians combines CBT with physiological interventions like biofeedback and neurofeedback, and nervous system regulation techniques when anxiety involves strong physical components that cognitive work alone doesn’t address. This integrative approach recognizes that anxiety lives in both your mind and body, requiring treatment that targets both systems.
Where to go from here
You now understand how cognitive behavioral therapy for anxiety targets the thoughts, feelings, and behaviors that maintain your symptoms. This treatment gives you practical tools you can use immediately, from cognitive restructuring and exposure exercises to behavioral experiments that test your anxious predictions against reality. The research backing CBT is solid, the techniques are learnable, and most people see meaningful improvement within three to four months of consistent work. Starting therapy requires finding a provider who matches your needs and circumstances. At Integrative Psychology, clinicians combine CBT with complementary approaches like biofeedback and mindfulness techniques when anxiety involves strong physiological components. The collaborative model means you actively participate in building skills rather than passively receiving treatment. Whether you schedule an in-person session or use secure telehealth services, taking that first step moves you from reading about anxiety treatment to actually experiencing relief.
April 24, 2026