Make an Appointment: (339) 707-5236 | info@integrativepsychology.com
integrative psychology, PC
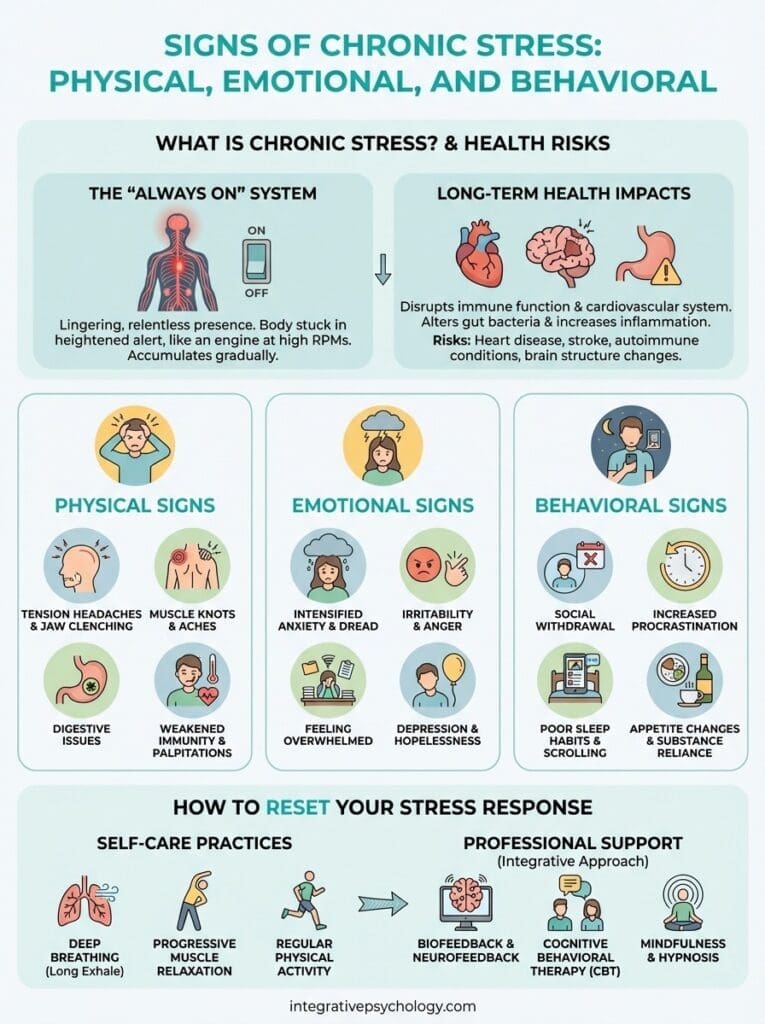
Signs Of Chronic Stress: Physical, Emotional, And Behavioral

Your body has been sending you messages. Maybe it’s the tension headaches that won’t quit, the sleep that never feels restorative, or the irritability that’s become your default setting. These could all be signs of chronic stress, your nervous system’s way of signaling that something needs to change.
Unlike acute stress, which resolves once a threat passes, chronic stress lingers. It rewires your brain, disrupts your hormones, and shows up in symptoms you might not immediately connect to stress at all. Digestive issues, frequent colds, difficulty concentrating, these aren’t random complaints. They’re often your body’s alarm system working overtime.
At Integrative Psychology, we work with adults whose chronic stress has started affecting both their mental and physical health. Our integrative approach, combining evidence-based psychotherapy with physiological interventions like biofeedback and neurofeedback, addresses stress at multiple levels. Understanding your warning signs is the first step toward meaningful change. This article breaks down the most common physical, emotional, and behavioral indicators of chronic stress, so you can recognize what’s happening and take informed action.
What chronic stress looks like
Chronic stress doesn’t announce itself with a single dramatic event. Instead, it accumulates gradually, showing up as a persistent hum of tension that colors your entire experience. You might notice that your shoulders never fully relax, or that you’re constantly bracing for the next problem. The physical sensations blend into your baseline until you forget what calm actually feels like.
When stress becomes constant
The defining characteristic of chronic stress is its relentless presence. Your body stays in a heightened state of alert, as if you’re perpetually preparing for a threat that never resolves. This differs fundamentally from acute stress, where your nervous system activates, handles a specific challenge, and then returns to baseline. With chronic stress, your system gets stuck in the “on” position.
Your stress response was designed for short bursts, not marathon sessions. When it runs continuously, every system in your body pays the price.
Think of it like running your car engine at high RPMs constantly. Eventually, something breaks down. Your adrenal glands keep pumping out cortisol. Your muscles maintain tension. Your mind stays vigilant, scanning for problems even during moments that should be restful.
Common patterns in daily life
You’ll recognize chronic stress in how it reshapes your routines. Maybe you wake up already feeling exhausted, regardless of how many hours you slept. You might find yourself checking your phone compulsively, unable to disconnect from work or responsibilities. Small inconveniences trigger disproportionate reactions, like getting unreasonably angry when someone cuts you off in traffic.
Physical sensations become background noise. That knot in your stomach before important meetings? It’s there all the time now. The jaw clenching you used to notice only during deadlines happens throughout the day. You compensate by drinking more coffee, skipping workouts you don’t have energy for, or using alcohol to finally wind down at night.
Your relationships shift too. Friends mention you seem distant or on edge. You cancel plans because you’re too drained to socialize. Simple decisions, like what to make for dinner, feel overwhelming. These aren’t character flaws. They’re signs of chronic stress wearing down your capacity to function at your normal level.
Why chronic stress matters for your health
Chronic stress doesn’t just make you feel bad. It fundamentally alters how your body functions, creating a cascade of physiological changes that increase your risk for serious health problems. When your stress response stays activated for weeks, months, or years, it becomes a primary driver of disease rather than a protective mechanism.
The cascade effect on your body systems
Your stress hormones, particularly cortisol, influence nearly every system in your body. Elevated cortisol disrupts your immune function, making you more susceptible to infections and slowing wound healing. It affects your cardiovascular system, raising blood pressure and heart rate in ways that strain your heart over time. Your digestive system also takes a hit, as stress redirects blood flow away from digestion and alters your gut bacteria.
The signs of chronic stress show up in lab work too. You might see elevated blood sugar levels as cortisol interferes with insulin sensitivity, increasing diabetes risk. Your cholesterol profile can worsen. Inflammation markers rise throughout your body, creating the perfect environment for chronic conditions to develop.
When your body treats every day like an emergency, it sacrifices long-term health for short-term survival.
Long-term health risks
Research connects prolonged stress exposure to increased risk of heart disease, stroke, and autoimmune conditions. Your brain structure actually changes, with chronic stress shrinking the hippocampus (crucial for memory) while enlarging the amygdala (your fear center). This makes you more reactive to future stressors and less able to regulate your emotions effectively. These aren’t minor inconveniences. They’re measurable biological changes that compound over time.
Physical signs of chronic stress
Your body speaks in physical symptoms when stress becomes chronic. These manifestations aren’t imaginary or exaggerated. They’re measurable physiological responses to your nervous system running on overdrive. You might dismiss them as separate issues, seeing a headache as just a headache or digestive problems as purely dietary, but they often connect to your stress load in ways that become obvious once you recognize the pattern.

Your body’s warning signals
The most common physical signs of chronic stress show up in predictable locations throughout your body. Tension headaches become frequent companions, often starting at your neck and radiating upward. Your jaw aches from grinding your teeth at night, something you might only discover when your dentist points out the wear. Muscle tension settles into your shoulders, neck, and back, creating knots that massage therapists comment on immediately.
Sleep disturbances rank among the most debilitating symptoms. You either struggle to fall asleep because your mind won’t stop racing, or you wake repeatedly throughout the night, never reaching the restorative deep sleep stages your body needs. Fatigue becomes constant, even after a full night in bed, because stress hormones disrupt your sleep architecture.
Your body can’t distinguish between real danger and perceived threats. It responds to work deadlines with the same physiological cascade it would use to escape a predator.
Chronic pain and tension patterns
Beyond headaches, you might experience unexplained body aches that move around or persist despite treatment. Digestive issues like nausea, diarrhea, or constipation appear seemingly without cause. Your immune system weakens, leading to frequent colds or infections that linger longer than they should. Some people develop skin problems like eczema flare-ups or hives. Heart palpitations and chest tightness prompt emergency room visits, only to have tests come back normal, indicating stress rather than cardiac disease as the culprit.
Emotional and behavioral signs of chronic stress
While physical symptoms often send you to a doctor, the emotional and behavioral signs of chronic stress can be harder to identify as stress-related. You might attribute mood changes to circumstances or personality rather than recognizing them as stress responses that require attention. These psychological shifts often appear gradually, making them easy to rationalize or ignore until they significantly impact your relationships and daily functioning.

Emotional shifts that signal stress overload
Your emotional landscape changes when stress becomes chronic. Anxiety intensifies beyond situational worry, showing up as generalized dread that colors your entire day. Irritability becomes your default setting, where minor frustrations trigger disproportionate anger or snapping at people you care about. You might notice persistent feelings of being overwhelmed, even when your actual workload hasn’t changed. Depression symptoms emerge, including loss of interest in activities you once enjoyed and a pervasive sense of hopelessness about the future.
Your emotional reactions aren’t character flaws. They’re your brain’s way of signaling that your stress load exceeds your current coping capacity.
Behavioral changes that compound the problem
Stress drives behavioral patterns that often worsen your situation. You might withdraw from social connections, canceling plans because you feel too drained or anxious. Procrastination increases as your overwhelmed brain seeks short-term relief by avoiding challenging tasks. Sleep habits deteriorate, with many people staying up too late scrolling through phones to feel a sense of control. Appetite changes swing both directions, either stress-eating for comfort or forgetting to eat entirely. You rely more heavily on alcohol, caffeine, or other substances to manage your emotional state, creating dependencies that add another layer of health consequences.
How to reset your stress response
Breaking the cycle of chronic stress requires deliberate intervention, not just wishful thinking or waiting for circumstances to improve. Your nervous system needs specific practices that signal safety and downregulate your stress response. These aren’t quick fixes, but concrete strategies that rewire how your body responds to daily pressures.
Physiological interventions that work
Techniques that directly target your nervous system produce measurable changes in stress hormones and heart rate variability. Deep breathing exercises, particularly those that extend your exhale longer than your inhale, activate your parasympathetic nervous system and counteract the fight-or-flight response. Progressive muscle relaxation teaches you to recognize and release the physical tension that accompanies stress. Regular physical activity metabolizes excess stress hormones while releasing endorphins that improve mood.
Your body can’t maintain a stress response when you’re breathing deeply and relaxing your muscles. These practices give your nervous system permission to stand down.
Professional support for lasting change
When the signs of chronic stress persist despite your efforts, specialized treatment becomes necessary. At Integrative Psychology, our clinicians combine evidence-based approaches like Cognitive Behavioral Therapy with physiological tools including biofeedback and neurofeedback, which train your nervous system to regulate more effectively. These interventions address stress at both the cognitive and biological levels, creating sustainable changes rather than temporary relief. Mindfulness-based therapies like Acceptance and Commitment Therapy help you develop a different relationship with stress, while techniques like clinical hypnosis and Cranial Electrotherapy Stimulation directly calm an overactive nervous system.
What to do next
Recognizing the signs of chronic stress gives you crucial information about what your body and mind need. You’ve likely identified several symptoms that match your experience, and that awareness itself represents an important first step toward change. Ignoring these warning signals allows stress to compound, creating deeper health consequences over time.
Start by choosing one or two practical strategies from this article that feel manageable. Maybe you commit to a daily breathing practice or schedule that workout you’ve been postponing. Small, consistent actions create momentum. Track your symptoms for a week to identify patterns in when they worsen or improve.
If your stress symptoms persist or interfere with your daily functioning, professional support makes a measurable difference. The team at Integrative Psychology combines traditional therapy with evidence-based physiological interventions designed specifically for adults dealing with chronic stress. You deserve specialized care that addresses both the mental and physical dimensions of stress.
April 28, 2026